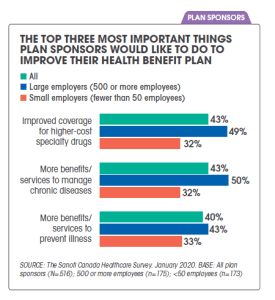
 A growing concern for health benefit plan sponsors continues to be the sustainability of drug plans heading into 2021. Specifically, employers are concerned about the rising costs of higher-cost specialty drugs for chronic disease management. Large employees with 500 or more employees in particular place this as one of their top three things they would like to do for their health plan: Improve coverage for higher-cost specialty drugs.
A growing concern for health benefit plan sponsors continues to be the sustainability of drug plans heading into 2021. Specifically, employers are concerned about the rising costs of higher-cost specialty drugs for chronic disease management. Large employees with 500 or more employees in particular place this as one of their top three things they would like to do for their health plan: Improve coverage for higher-cost specialty drugs.
Several factors are at play here. The Canadian boomer cohort is aging, and so chronic disease is increasing in that group, but often those chronic illnesses have an earlier onset for people in the 35-55 age group. Many chronic diseases can be managed well but that requires patients’ access to high cost drugs.
But there is no one-size-fits-all benefits plan. Every workplace will have diverse employee demographics. The COVID-19 pandemic may impact employees across the demographic spectrum into 2021 until vaccines are widely available. Employees who contract COVID-19 may need to access their health benefits plans to get the immediate and ongoing treatment they will require to fully recover and return to work.
According to the 2020 Sanofi Canada Healthcare Survey, 88% of health plan sponsors agree they would like to see their benefit plan to do more to support plan members with chronic disease.
The Sanofi survey also found that in the majority of plans sponsors, their top five concerns are:
- Drug Plan Sustainability – 45%
- Dental Plan Sustainability – 42%
- Absence/Disability – 32%
- Use of paramedical benefits – 29%
- Fraud – 28%.
What steps can plan sponsors take as we head into 2021?
Focus on taking a data driven approach to analyzing claims for drugs, paramedical services, disability claims and use of other benefits. Understand how chronic illness drug benefits usage has been affecting your organization’s claims, and then investigate how to offer specific programs and services for chronic disease management.
Of interest is the fact that a recent survey by Sun Life showed that 60% of Canadians reported a negative impact on their health because of the pandemic. Mental illness is a comorbidity for many other chronic conditions, which is why, when looking at the bigger picture of creating plans to address chronic illness, mental health has to become a larger priority.
At Health Risk Services, we have been assisting plan sponsors in the modification of their current plans to adapt to the changing realities in public health, especially with the pandemic, but also the costs of drugs, and the rise of mental illness. We can assist you as well in making these plan changing decisions! Schedule a Complimentary Consultation with Health Risk Services…we will empathize, educate, and empower you and your team into 2021!
Health Risk Services
403-236-9430













